Does Introducing Solids Early Help Your Baby Sleep? New research suggests yes but. . .
Parents often wonder if solids will help baby sleep better. A new research study was released this week about solid food and baby sleep, and is already generating headlines:
The study is entitled “Association of Early Introduction of Solids With Infant Sleep”, with a lead author of Michael R Perkin. (Perkin, M. R. et al. Association of Early Introduction of Solids With Infant Sleep: A Secondary Analysis of a Randomized Clinical Trial. JAMA Pediatr e180739–e180739 (2018). doi:10.1001/jamapediatrics.2018.0739).
But will solids help your baby sleep better? The question is more complicated that it seems.
The Background
Many new parents are told that the sooner they start solid foods, the sooner their baby will sleep through the night. However, the very limited research available has suggested that this is not actually the case.One study showed that adding rice cereal to formula at either five weeks or four months of age did not help babies sleep through the night.
The problem is, most babies will start sleeping through the night anyway around 4-6 months of age, when solids are commonly introduced. Introducing solid food early has been controversial, with concerns that it may be associated with the development of food allergy or obesity, and that it may adversely affect breastfeeding
Our Current Story: The EAT Study
The Enquiring About Tolerance study was designed to see if starting selected solid foods in infants prevents food allergies. You can read more about he results of the initial trial here.
This current publication is what is called a “secondary analysis”— meaning that they took other data collected during the study and analyzed it looking specifically at sleep information. The good think about secondary analyses is that they the ensure that every bit of information collected during (very expensive) clinical trials is made available. The downside is that the data is often used to answer questions that the study was not designed to answer. Thus, the authors sometimes lack important information when writing up their result. For example, this study was designed to look at the development of food allergy as a primary endpoint. Sleep information was collected to supplement this.
What are the sleep results from the trial?
Thirteen hundred and three children were enrolled, with 1225 having complete sleep data. Half were in the Early Introduction of food Group (EIG) and half were in the Standard Intervention Group (SIG— exclusively breastfed). There were three primary findings. (Note that all images are taken from the article above).
- Infants in the EIG group slept longer than infants in the SIG group— by about 16 minutes per night at six months of age, when the difference in sleep amounts was maximal.
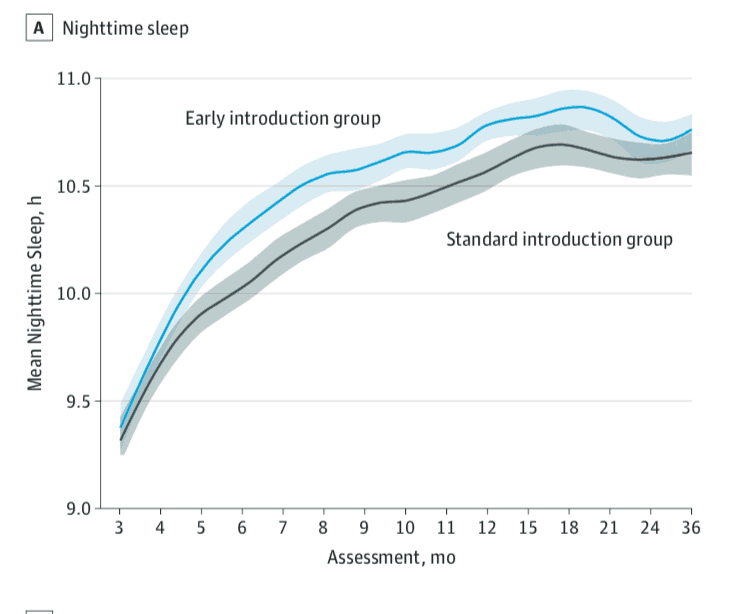
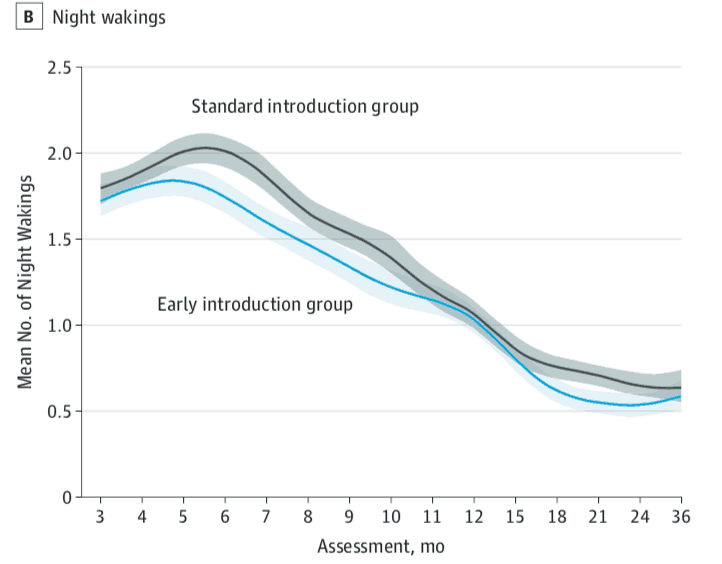
- The night time awakenings decreased from 2.01 to 1.74 per night. This translates to about one fewer awakening every four nights, or a little bit less than two fewer awakenings per week.
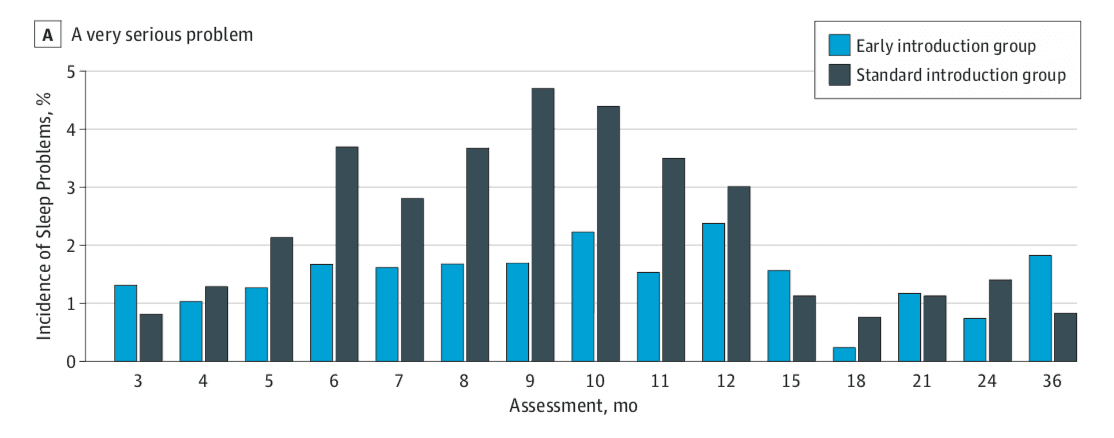
- “Very serious sleep problems” were reported more frequently in the SIG vs. EIG group. Note that this is based on parental report— not medical diagnoses. Specifically, the parents were asked, “Do you consider your child’s sleep as a problem?” With the options to answer being “A very serious problem”, “A small problem”, or “Not a problem at all”.
The problem with these results
My colleague Monica Ordway (shout out to her on Twitter here) is an expert in both lactation and sleep disorders in children. She’s concerned about the conclusions of the authors as presented in this study.
Here’s the points she makes about the data analyzed in the study:
- “The authors controlled for sleep location at baseline because, as expected based on my research findings to date and findings of others, sleep location affects sleep characteristics like night waking. However, they did not control for sleep location after randomization. It is possible that the babies sleep location changed when they began to eat solids and it is plausible that sleep location contributed significantly to the statistical models.. I would hypothesize that the EIG (early feeding group) parents also separated earlier from their children during bedtime than the SIG (late feeding group) parents who continued to exclusively breastfeed. If that were the case then the message from the sec-ondary analysis would be that babies who sleep independently sleep longer and with fewer night wakings, regardless of feeding method.”
- “There is no mention of the rapid metabolism of breast milk – it is logical that adding calories (especially the dense calories in thehigher protein/fat food items that were introduced) with longer metabolism rates will result in longer sleeping. Introduction of solids at this early age may inadvertently interrupt the supply and demand natural rhythm of breastfeeding and result in early termi-nation of breastfeeding”
- “Their reporting of “serious sleep problems” is mis-represented. The proper way to report their findings would be to say that there were fewer parents who reported that they believed their children’s sleep habits were a serious problem.”
Here’s my read on the issues Dr. Ordway raises. Essentially, the families sleep practices were surveyed when the subjects were surveyed monthly from 3-12 months of age then every 3 years of age until age 3. However, where the baby sleeps is only considered from the initial survey. Research conducted at our center (and others) has shown that babies who sleep in a different room from parents are more likely to sleep through the night than if they room- or bed-share.
The problem is this. Breast milk is digested much more quickly than other foods. So introducing solid food may be keeping kids sated longer. Or, alternatively, moms who know that the baby is receiving solid food may be more likely to change where the baby sleeps or sleep train because they think that solid foods make babies sleep better.
I’m not saying that the results reported are not true— my concern is that important information about where and how the babies in the study fall asleep was not included in the analysis.
What’s the downside to starting food early in infants?
Both the American Academy of Pediatrics and the World Health Organization recommend exclusive breastfeeding for the first six months of life as it seems to offer the best benefits for mother and baby. Certainly, starting food early may result in decreased milk supply (especially if it reduces nursing at night).
I’m not a lactation expert, but I briefly reviewed the evidence for exclusive breastfeeding for six months (versus four months). A Cochrane review from 2012 suggests that the main benefit is a reduction in respiratory and gastrointestinal illnesses in infants, as well and prolonged lactation amenorrhea (which delays pregnancy in the mother, thus increasing the time between children and reducing the risk of prematurity). These are important goals, but perhaps more significant in the third world than in the US or Europe.
However, continued breastfeed is clearly an important goal for maternal and child health. Introducing food at three months of age may actually place a mother’s milk supply in particular jeopardy, for two reasons:
- After several months of nursing, maternal prolactin levels decrease, which can lead to a decrease in milk supply.
- In the United States, most working moms have to return to work around three months after birth. This is a challenging time to continue breast feeding as these moms will need to transition to pumping more. This is a difficult and stressful time which can lead to a further reduction in milk supply.
Thus, the concern is that adding solid foods at three months of age can put breastfeeding in jeopardy.
So Will Solids Help Baby Sleep Better?
The answer seems to be a qualified yes BUT the downside seems greater than the upside here. To me, the biggest reason to do so seems to be reduce the risk of food allergy in children at high risk of food allergy (infants with severe eczema, egg allergy, etc) may benefit from peanut introduction between 4-6 months of age. (Here’s the American Academy of Pediatrics recommendations if you want to know more). Clearly, this is something you should do in consultation with your pediatrician.
I do not think that the very modest benefits noted in this study suggest that you should introduce solids at three months of age to improve your child’s sleep. (Trust me, I understand that those extra few minutes of sleep sound tempting).
So what should you do instead?
Dr. Ordway notes that you can get similar benefits by changing your nursing strategies at night, “such as pumping and skimming off higher fat content milk for night feedings, ensuring mom is breastfeeding on one side and “emptying” that side before going to the next.” If you have questions about this, I would recommend that you work with your pediatrician or a lactation specialist.
If you need further help, check out:
Eight Ways to Avoid Sleep Training Your Baby
How to Stop Night Feeding and Sleep Better
Sleep Training Techniques for the Exhausted Parent
Tell me, what are your questions about this topic. Are you tempted by the results of this study? If you have older children, would this news around this study have tempted you to start solids earlier?
Originally published July 2018. Last reviewed/updated by Dr. Craig Canapari, MD in July 2018
No spam, no sharing to third party. Only you and me.